Search
- Page Path
- HOME > Search
Original Article
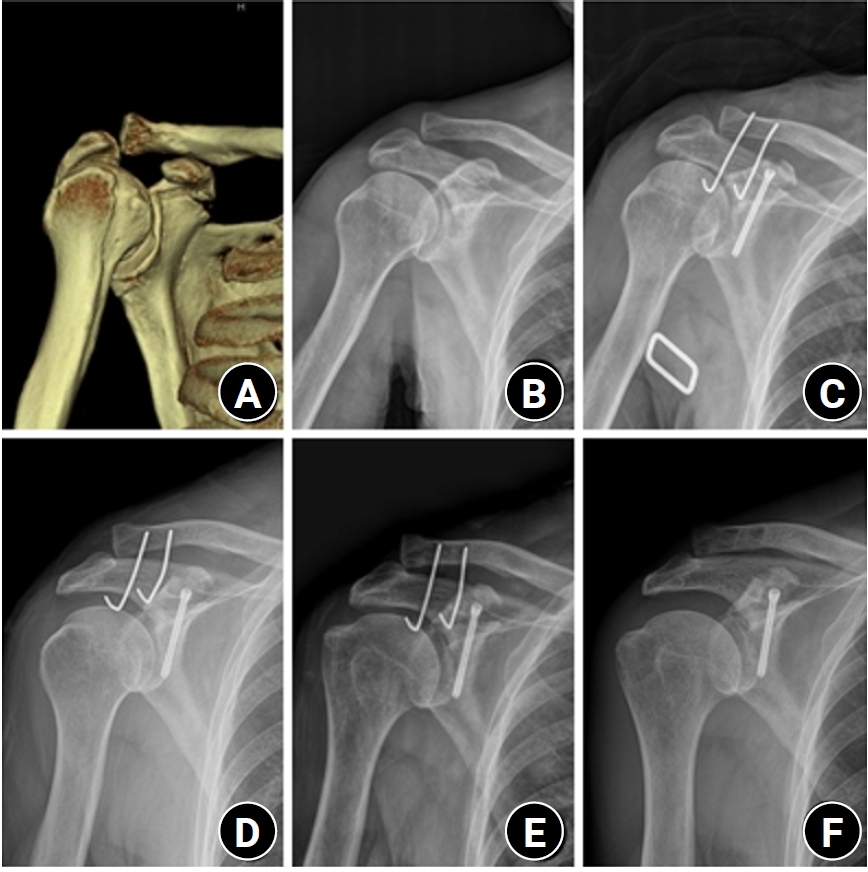
- Surgical outcomes of the coracoid process fracture associated with the acromioclavicular joint injury in Korea: a case series
- Dongju Shin, Sung Choi, Sangwoo Kim, Byung Hoon Kwack
- J Musculoskelet Trauma 2026;39(1):54-61. Published online January 14, 2026
- DOI: https://doi.org/10.12671/jmt.2025.00346
-
 Abstract
Abstract
 PDF
PDF - Background
Excluding technical reports and isolated case reports, there are no published studies evaluating coracoid process fixation with or without an acromioclavicular joint (ACJ) stabilization procedure for coracoid process fractures associated with ACJ injury. The purpose of this study was to assess the surgical outcomes of coracoid process fractures associated with ACJ injuries and to determine the usefulness of coracoid process fixation with or without an ACJ stabilization procedure.
Methods
From February 2006 to December 2015, patients with coracoid process fractures associated with ACJ injuries were enrolled. Radiological and clinical outcomes were analyzed in 12 patients who underwent coracoid process fixation with or without an ACJ stabilization procedure. A 3.5-mm cannulated screw with a washer or a 3.0-mm headless compression screw was used for coracoid process fixation, and either a clavicle hook plate or Kirschner (K)-wires were used for ACJ injuries when additional fixation was necessary.
Results
Bone union was achieved in 11 patients (91.7%), while one case was determined to be a nonunion at 6 months. Radiological union occurred at an average of 3 months (range, 1.5–4 months) in all patients except the nonunion case. At the final follow-up, the average clinical scores were a visual analogue scale (VAS) pain score of 1.5 (range, 0–4) and a UCLA score of 30.9 (range, 28–35). Clinical outcomes were satisfactory in all patients, including the patient with nonunion.
Conclusion
The clinical and radiological outcomes of treating coracoid process fractures associated with ACJ injuries using coracoid process fixation with or without ACJ stabilization were favorable. A cannulated screw with a washer and clavicle hook plate fixation may provide sufficient stability for both the coracoid process fracture and the ACJ injury when feasible. Level of evidence: IV.
- 423 View
- 13 Download

Case Report
- Irreducible Ankle Fracture Dislocation due to Dislocated Tibialis Posterior Tendon - A Case Report -
- Seungyup Shin, Bum-Soo Kim, Ji-Won Lee, Euisun Yoon
- J Korean Fract Soc 2023;36(2):52-56. Published online April 30, 2023
- DOI: https://doi.org/10.12671/jkfs.2023.36.2.52
-
 Abstract
Abstract
 PDF
PDF - An irreducible ankle dislocation is a rare injury. The cause is a dislocation of the distal fibula anteriorly or posteriorly or the insertion of soft tissue, such as the deltoid ligament or posteromedial tendon. The tibialis posterior tendon can be dislocated through distal tibiofibular diastasis and prevent reduction of the ankle joint. The authors experienced anterolateral ankle fracture dislocation with a diastasis of the distal tibiofibular joint, and reduction was impossible because of impingement of the tibialis posterior tendon dislocated anteriorly through the distal tibiofibular diastasis. This paper reports the treatment of this injury.
- 683 View
- 15 Download

Review Articles
- Perilunate Dislocation and Perilunate Fracture-Dislocation
- Jung Il Lee
- J Korean Fract Soc 2022;35(3):114-119. Published online July 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.3.114
-
 Abstract
Abstract
 PDF
PDF - Perilunate dislocations and perilunate fracture-dislocations are one of the most severe forms of wrist injuries and are generally caused by high-energy trauma such as falls from a height or traffic accidents. Prompt recognition and immediate, gentle closed reduction are critical, but diagnosis can often be missed at the initial presentation. The current standard management is open reduction, ligamentous and bony repair, and supplemental fixation for the protection of the repair. The pathomechanics of the injury, diagnosis by plain wrist radiographs, closed reduction techniques, current surgical treatments, and complications are presented in this review.
- 768 View
- 10 Download

- Current Treatment of Calcaneal Fractures and Dislocation
- Dae Jin Nam, Sung Hyun Lee
- J Korean Fract Soc 2022;35(2):74-82. Published online April 30, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.2.74
-
 Abstract
Abstract
 PDF
PDF - Calcaneal fractures are the most common fractures occurring in the tarsal bone. In the past, surgical treatments were not preferred because they were accompanied by severe comminution and soft tissue complications. In recent years, there have been great advancements in the treatment of calcaneal fractures owing to the development of new surgical techniques and instruments. However, a standard treatment method has not yet been established. In this review article, we summarize the latest information on the indications and treatment methods of calcaneal fractures.
- 687 View
- 15 Download

- Treatment of Ankle Fracture and Dislocation
- Chan Kang
- J Korean Fract Soc 2022;35(1):38-49. Published online January 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.1.38
-
 Abstract
Abstract
 PDF
PDF - Ankle fractures are the most common type of foot and ankle fracture injury. Several types of fractures occur in the ankle structures (medial malleolus, lateral malleolus, posterior malleolus, and Chaput’s tubercle) with various mechanisms and extent of fracture force. Moreover, fractures can be accompanied by other injuries, such as distal tibiofibular syndesmotic injury, medial deltoid ligament rupture, and lateral ligament complex rupture. Ankle dislocation can be accompanied when an injury is caused by a greater fracture force. Non-surgical treatments or combined surgeries may be performed depending on the mechanism and fracture type. Generally, a stable fracture maintaining anatomical reduction is treated conservatively, but surgical treatment is performed when this is not the case. Furthermore, surgeries for stable fractures can be offered when the patients demand early weight bearing due to their occupation, age, and performance state. Restoring the ankle mortise in its anatomical shape before the injury and starting early rehabilitation for functional recovery simultaneously until a union is achieved is important. Traumatic arthritis can occur if the treatment focuses only on fractures and neglects ligament injuries, such as distal tibiofibular syndesmotic injury and medial deltoid ligament rupture. Shortening, angular deformation, and rotational deformation of the fibular promote the progression of traumatic ankle arthritis in the long term, which may further cause chronic ankle pain. An overlooked displaced posterior malleolus fracture also causes traumatic arthritis through anteroposterior instability of the ankle joint.
- 1,246 View
- 48 Download

Case Report
- Axillary Artery Rupture after Shoulder Dislocation That Was Treated with a Self-Expanding Stent - A Case Report -
- HaengJin OHE, Daehyun Hwang, Inkeun Park, Minki Lee, Jun-Ku Lee
- J Korean Fract Soc 2020;33(4):217-221. Published online October 31, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.4.217
-
 Abstract
Abstract
 PDF
PDF - raumatic shoulder dislocations are one of the most common major dislocations in the general population. Injury to major vessels is rarely reported as a complication of shoulder dislocations. This case report presents the traumatic dissection of the axillary artery after a simple shoulder dislocation that was managed successfully with the placement of a self-expanding stent. With the clinical manifestations of a brachial plexus injury and progressive vascular compromise in the affected arm, a major vascular injury was detected on an angiogram, and a self-expanding stent was deployed. Through immediate diagnosis and prompt intervention, serious complications, such as hypovolemic shock and even death, were averted, ultimately achieving a favorable patient outcome.
- 1,469 View
- 8 Download

Original Article
- Risk Factors Affecting the Early Complications of Femoral Head Fractures
- HoeJeong Chung, Jin-Woo Lee, Dong Woo Lee, Hoon-Sang Sohn
- J Korean Fract Soc 2020;33(4):204-209. Published online October 31, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.4.204
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study analyzed the prognostic factors in patients with femoral head fractures by comparing two groups with and without complications.
Materials and Methods
A retrospective study was performed on femoral head fracture patients who visited two different level-1 trauma centers from January 1, 2014 to June 30, 2018. Thirty-three patients with a follow-up period of more than one year were included. Early complications were defined as fair or poor in the Thompson–Epstein clinical evaluation criteria and grades 3 or 4 in the Kellgren– Lawrence classification within one year after the fracture. The patients were divided into two groups, with and without early complications. Statistical analysis was performed for the nominal variables with a Fisher’s exact test and continuous variables using a Mann–Whitney U test.
Results
Nine patients (27.3%) had early complications, and there were no significant differences according to age, sex, treatment method, combined fractures, Pipkin classification, and AO/OTA classification between the two groups.
Conclusion
The prognosis in femoral head fractures is difficult to predict. Therefore, the validation of existing classifications or a new classification is necessary.
- 633 View
- 1 Download

Case Reports
- Femoral Head Fracture with Hip Dislocation Treated by Autologous Osteochondral Transfer (Mosaicplasty) - A Case Report -
- Eui-Sung Choi, Hyun-Chul Shon, Ho-Seung Jeong, Jae-Young Yang, Seok-Hyun Hong, Byung-Hyun Ahn
- J Korean Fract Soc 2020;33(2):96-100. Published online April 30, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.2.96
-
 Abstract
Abstract
 PDF
PDF - Femoral head fractures combined with hip dislocation are very rare injuries. In most cases, they result from high-energy trauma to the hip or lower extremity during traffic accidents. Various therapy options have been suggested to treat these injuries. Especially, different joint-preserving surgical options have been described for the treatment of traumatic osteochondral injury of the femoral head in young, active patients. In this report, we present a case that a traumatic osteochondral lesion to the femoral head after hip dislocation was treated with osteochondral autografts (OATS) from the non-weight-bearing area of the ipsilateral inferior femoral head through a surgical hip dislocation. After 1 year, the clinical and radiological outcome was satisfactory with no evidence of posttraumatic osteoarthritis and no pain of patients.
-
Citations
Citations to this article as recorded by- Femoral head fracture with large crushed defect in weight-bearing area treated with autologous osteochondral transplantation (repositionplasty): A case report
Hyun-Chul Shon, Eic-Ju Lim, Jae-Young Yang, Seung-Jun Jeon
Medicine.2022; 101(52): e32569. CrossRef
- Femoral head fracture with large crushed defect in weight-bearing area treated with autologous osteochondral transplantation (repositionplasty): A case report
- 825 View
- 2 Download
- 1 Crossref

- Treatment of Neglected Proximal Interphalangeal Fracture Dislocation Using a Traction Device: A Case Report
- Yongun Cho, Jai Hyung Park, Se Jin Park, Ingyu Lee, Eugene Kim
- J Korean Fract Soc 2019;32(4):222-226. Published online October 31, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.4.222
-
 Abstract
Abstract
 PDF
PDF - This paper reports the use of a traction device for the treatment of neglected proximal interphalangeal fracture dislocations. A 44-year-old man with a fracture dislocation of a right ring finger proximal interphalangeal joint was admitted 17 days after the injury. Closed reduction and external fixation were performed using a dynamic traction device and C-arm under a brachial plexus block. Passive range of motion exercise was started after two weeks postoperatively and active range of motion exercise was started after three weeks. The traction device was removed after five weeks. No infection occurred during the traction period. No subluxation or displacement was observed on the X-ray taken two months postoperatively. The active range of motion of the proximal interphalangeal joint was 90°. The patient was satisfied with the functional result of the treatment with the traction device. The dynamic traction device is an effective treatment for neglected fracture dislocations of the proximal interphalangeal joint of a finger.
- 1,751 View
- 9 Download

Review Article
- New Injury Mechanism and Treatment Algorithm of Posterior Elbow Dislocation
- In Hyeok Rhyou
- J Korean Fract Soc 2019;32(1):61-71. Published online January 31, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.1.61
-
 Abstract
Abstract
 PDF
PDF - Although the concept of a single elbow dislocation mechanism, in which all dislocations start from the lateral side of the elbow joint and progress to the medial side, has never been able to explain the various conflicting experimental and clinical observations thus far, new studies and proposals for a valid mechanism have not been reported. The new proposal for posteromedial and posterolateral dislocation of the elbow joint according to the authors' study and the new treatment algorithm based on this new study can explain the various clinical and experimental results that have been difficult to explain, and provide a reasonable approach to the treatment of elbow dislocations.
- 1,853 View
- 16 Download

Original Article
- Surgical Outcomes of the Monteggia Type 2 Fracture Dislocation in Adults
- Sung Choi, Daegeun Jeong, Youngsoo Byun, Taehoe Gu, Sungsoo Ha, Dongju Shin
- J Korean Fract Soc 2019;32(1):6-13. Published online January 31, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.1.6
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
This study examined clinical outcomes of Monteggia fracture type 2, which is the most common in adults with a high rate of accompanied injuries.
MATERIALS AND METHODS
From June 2004 to November 2015, a retrospective study was performed on 12 patients diagnosed with Monteggia fracture type 2 with a follow-up period of at least 6 months after surgery. The clinical outcomes were evaluated using the Mayo elbow performance score (MEPS), and the existence of accompanied injures, radiological result, and complications were analyzed.
RESULTS
Posterior instability was confirmed in all patients and accompanied fractures were detected in 9 patients (75.0%) on the radial head, whereas 10 patients (83.3%) were found on the coronoid process. The average arc of motion was 107° (70°–130°) and the mean MEPS was 89 (45–100). Additional re-operation due to re-dislocation, radioulnar synostosis, elbow instability, ulna nonunion, and radial head nonunion were performed in 4 cases (33.3%).
CONCLUSION
The Monteggia fracture type 2 is more commonly associated with radial head fractures and coronoid process fractures rather than other types, which causes elbow instability. Because the rate of additional surgery due to complications is high, the treatment of Monteggia fracture type 2 requires careful assessments.
- 1,132 View
- 6 Download

Case Report
- Shoulder Quadruple Dislocation Fracture: Fracture of Glenoid Rim, Coracoid Process, Greater Tuberosity, Surgical Neck of Humerus Associated with Anterior Shoulder Dislocation: A Case Report
- Jae sung Yoo, Seong jun Kim, Seung gwan Park, Joong Bae Seo
- J Korean Fract Soc 2019;32(1):47-51. Published online January 31, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.1.47
-
 Abstract
Abstract
 PDF
PDF - Shoulder joint dislocation has the most common incidence rate compare compared to other joints. It is reported that shoulder Shoulder dislocation couldmay be associated with glenoid rim, greater tuberosity of humerus and coracoid process fracture. There were have only been 2 cases of anterior shoulder dislocation simultaneously combined with simultaneous glenoid rim, coracoid process, and humerus greater tuberosity fracture worldwide and no report reports in Korea. We present a case of quadruple fracture (glenoid rim, coracoid process, greater tuberosity, surgical neck of humerus) associated with anterior shoulder dislocation and treated successfully by open reduction. In addition, with we provide the injury mechanism, diagnosis, treatment procedure and discussion.
- 810 View
- 2 Download

Original Articles
- Clinical Features and Characteristics of Greater Tuberosity Fractures with or without Shoulder Dislocation
- Dong Wan Kim, Young Jae Lim, Ki Cheor Bae, Beom Soo Kim, Yong Ho Lee, Chul Hyun Cho
- J Korean Fract Soc 2018;31(4):139-144. Published online October 31, 2018
- DOI: https://doi.org/10.12671/jkfs.2018.31.4.139
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study was to compare the characteristics and clinical features of greater tuberosity fractures with or without a shoulder dislocation.
MATERIALS AND METHODS
A total of 108 cases of greater tuberosity fractures (56 cases with shoulder dislocation, 52 cases without shoulder dislocation) were reviewed retrospectively. Age, sex, side, injury mechanism, fracture displacement, fracture morphology, number of fracture fragments, main fragment size, treatment, and combined injuries were investigated.
RESULTS
The age, sex, side, injury mechanism, treatment, and combined injuries were similar in both groups (p>0.05). A statistically significant difference in fracture displacement, fracture morphology, number of fracture fragment, and main fragment size was observed between the two groups (p < 0.05).
CONCLUSION
In greater tuberosity fractures with a shoulder dislocation, the prevalence of fracture displacement was high and the depression type of fractures occurred frequently. In addition, the number and size of the fracture fragment increased. Therefore, an understanding of these fracture patterns will be helpful for deciding treatment and prognosis.
- 376 View
- 1 Download

- The Cause of Primary Reduction Failure in Hip Dislocation with or without Hip Fracture
- Hee Gon Park, Yong Eun Shin, Sung Hyun Kim
- J Korean Fract Soc 2017;30(1):9-15. Published online January 31, 2017
- DOI: https://doi.org/10.12671/jkfs.2017.30.1.9
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
A rapid and accurate reduction is important for hip dislocated patients to avoid various potential complications, including avascular necrosis of the femoral head. We analyzed hip dislocation cases, ones that particularly failed during the primary reduction trial.
MATERIALS AND METHODS
Eighty-seven patients with hip dislocation, who visited the emergency department between January 2007 and September 2015, were retrospectively analyzed. Of them, 68 patients were successfully treated in the first closed reduction trial, and the remaining 19 patients were unsuccessful. Of the 19 unsuccessful first trial, 12 patients were successfully treated in the second closed reduction; however, in the remaining 7 patients, open reduction was performed in the operation room with general anesthesia. Every closed reduction was practiced by at least 2 orthopedic doctors, and open reduction was performed by a single senior author.
RESULTS
The rate of first reduction failure was higher, with statistical significance, in patients aged under 50 years, male gender, and those with combined around hip fractures, including femoral head and acetabular fracture (p<0.05). In particular, the presence of impacted fracture fragment in the hip joint and large size of the impacted fracture fragment was highly related to the failure of second closed reduction trial requiring open reduction. Conversely, the method of reduction, Thompson-Epstein classification, Pipkin classification were not related to the failure of closed reduction statistically (p>0.05).
CONCLUSION
To evaluate the patients with hip dislocation, realizing the type of dislocation, presence of accompanied fracture, location and size of fracture fragment, age, as well as gender of patients is important. If the fracture fragment is impacted in the hip joint and the size of the fragment is large, then the operative treatment is considered, rather than the repetitive trial of closed reduction by constraint. -
Citations
Citations to this article as recorded by- Atypical and unclassifiable hip dislocation with capsule and labrum incarceration: a case report and review of the literature
Francis Zifa Pentèce Zengui, Moise Radam Ellah, Kevin Bienvenu Parfait Bouhelo-Pam, Arnauld Sledge Wilfrid Bilongo-Bouyou, Nevil Stève Ngona Gampio Mvili, Marius Monka
International Journal of Surgery Case Reports.2025; 135: 111879. CrossRef - Traumatic obturator dislocation of the hip joint
Z. F. Zengui, O. El Adaoui, M. Fargouch, O. Adnane, Y. El Andaloussi, M. Fadili
International Journal of Surgery Case Reports.2022; 93(C): 106983. CrossRef
- Atypical and unclassifiable hip dislocation with capsule and labrum incarceration: a case report and review of the literature
- 1,197 View
- 5 Download
- 2 Crossref

- A Comparison of Results between AO Hook Plate and TightRope for Acute Acromioclavicular Joint Dislocation
- Yong Gun Kim, Ho Jae Lee, Dong Won Kim, Jinmyoung Dan
- J Korean Fract Soc 2017;30(1):16-23. Published online January 31, 2017
- DOI: https://doi.org/10.12671/jkfs.2017.30.1.16
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of our study is to compare the radiographic and clinical outcomes with respect to acromioclavicular (AC) joint dislocation depending on the surgical method: Hook plate (HP) versus TightRope (TR).
MATERIALS AND METHODS
Between May 2009 and May 2012, 51 patients with Rockwood type III-V lesions received clinical and radiographic follow-up. Patients were divided into two groups according to the surgical methods (HP: n=32; TR: n=19). Radiological follow-up included comparative coracoclavicular distance (CCD) measurements as a percentage of the uninjured shoulder. For clinical follow-up, a standardized functional shoulder assessment with the Constant score, University of California at Los Angeles (UCLA) score, and Korea shoulder score (KSS) were carried out.
RESULTS
Comparing the functional results, no differences were observed between the two groups (Constant score: HP, 78.5; TP, 81.4; UCLA score: HP, 29.2; TP, 29.9; KSS: HP, 79.2; TP, 80.7). Time to restoration of the range of motion (ROM) above shoulder level was longer in the HP group than in the TR group. However, the ROM at 1 year postoperation and final follow-up revealed similar results between the two groups. The AC joints were well reduced in both groups, the CCD increased to 44.7% in the HP group and to 76.5% in the TR group at the final follow-up; however, no one was significantly superior to the others. Furthermore, there were 8 cases (25.0%) and 5 cases (26.3%) of AC joint arthritis in the HP group and TR group, respectively. However, the observed AC joint arthritis has a poor correlation between clinical symptom and radiological results in both groups.
CONCLUSION
Both HP and TR fixation could be a recommendable treatment option in acute unstable AC joint dislocation. Both groups showed excellent radiologic and functional results at the final visit. Moreover, there was no significant difference in statistics, except for the time to restoration of ROM above shoulder level. -
Citations
Citations to this article as recorded by- Suture-Button Fixation Outperforms Hook Plate in Functional Outcomes After Acromioclavicular Joint Dislocation
Murat Aşçı, Mete Gedikbaş
Bozok Tıp Dergisi.2025; 15(4): 477. CrossRef - Arthroscopic Treatment of Acromioclavicular Joint Dislocations
Du-Han Kim, Chul-Hyun Cho
Journal of the Korean Orthopaedic Association.2023; 58(5): 384. CrossRef - Combination of Clavicular Hook Plate with Coracoacromial Ligament Transposition in Treatment of Acromioclavicular Joint Dislocation
Aikebaier Tuxun, Ajimu Keremu, Pazila Aila, Maimaitiaili Abulikemu, Zengru Xie, Palati Ababokeli
Orthopaedic Surgery.2022; 14(3): 613. CrossRef
- Suture-Button Fixation Outperforms Hook Plate in Functional Outcomes After Acromioclavicular Joint Dislocation
- 2,794 View
- 8 Download
- 3 Crossref

Review Article
- Current Concepts of Fractures and Dislocation of the Hand
- Yong Cheol Yoon, Jong Ryoon Baek
- J Korean Fract Soc 2016;29(2):143-159. Published online April 30, 2016
- DOI: https://doi.org/10.12671/jkfs.2016.29.2.143
-
 Abstract
Abstract
 PDF
PDF - Fractures and dislocation of the hand is a body injury involving complex structures and multiple functions, which frequently occur as they represent 10%-30% of all fractures. Such fractures and dislocation of the hand should be treated in the context of stability and flexibility; and tailored treatment is required in order to achieve the most optimal functional performance in each patient since deformation may occur if not treated, stiffness may occur with unnecessarily excessive treatment, and both deformation and stiffness may occur coincidently with inappropriate treatment. Stable injuries can be fixed with splintage whereas surgery is actively considered for unstable injuries. In addition, surgeons should keep in mind that as the surgical intervention is done aggressively, aggressive rehabilitation must be followed in correspondence with the surgical intervention. Successful outcome requires effort to prevent any potential complication including nerve hypersensitivity and infection. Finally, it is also important that the patient to know that swelling, stiffness, and pain may last for a long period of time until the recovery of fractures and dislocation of the hand.
-
Citations
Citations to this article as recorded by- Current concepts in the management of phalangeal fractures in the hand
Hyun Tak Kang, Jun-Ku Lee
Journal of Musculoskeletal Trauma.2025; 38(3): 109. CrossRef - Current Concepts in Management of Phalangeal Fractures
Yohan Lee, Sunghun Park, Jun-Ku Lee
Journal of the Korean Fracture Society.2022; 35(4): 169. CrossRef
- Current concepts in the management of phalangeal fractures in the hand
- 1,440 View
- 26 Download
- 2 Crossref

Case Reports
- Iatrogenic Humeral Fracture during Reduction of Shoulder Dislocation: Two Cases Report
- Hyung Lae Cho, Hyoung Min Kim, Ki Bong Park, Tae Hyun Wang, Dong Hyun Lee
- J Korean Fract Soc 2016;29(1):50-54. Published online January 31, 2016
- DOI: https://doi.org/10.12671/jkfs.2016.29.1.50
-
 Abstract
Abstract
 PDF
PDF - Shoulder dislocation is the most common dislocation presenting to the emergency department. In old age, the attempt of closed reduction is made with caution in order to prevent iatrogenic fracture around the shoulder. We report two cases of iatrogenic fractures of humeral shaft and anatomical neck in female patients older than 70 years old, which occurred during the manual closed reduction. One patient was proved as first-time and the other was recurrent. In addition, the second case had a massive irreparable rotator cuff tear. Those patients were treated successfully with humeral nailing and reverse total shoulder arthroplasty, respectively.
- 495 View
- 5 Download

- Irreducible Open Dorsal Dislocation of the Proximal Interphalangeal Joint: A Case Report
- Youn Tae Roh, Il Jung Park, Hyoung Min Kim, Jae Young Lee, Sung Lim You, Youn Soo Kim
- J Korean Fract Soc 2015;28(1):65-70. Published online January 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.1.65
-
 Abstract
Abstract
 PDF
PDF - Dorsal dislocation of the proximal interphalangeal joint is a common injury in the orthopedic department. In most cases, the joint is reduced simply by closed manipulation. However, in rare cases, the joint is not reducible by closed manipulation, therefore, surgery is required. We report on a case of irreducible open dorsal dislocation of the proximal interphalangeal joint which was surgically treated. Because the flexor tendon interposed between the head of the proximal phalanx and the base of the middle phalanx, we could reduce the joint only after repositioning of the flexor tendon.
- 534 View
- 2 Download

- Peroneus Tendon Dislocation Associated with Fracture of Lateral Process of Talus: A Case Report
- Youn Soo Hwang, Sung Jun Jo, Kwang Yeol Kim, Hyung Chun Kim, Dong Seon Kim
- J Korean Fract Soc 2014;27(3):222-226. Published online July 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.3.222
-
 Abstract
Abstract
 PDF
PDF - Traumatic peroneal tendon dislocation in association with fracture of the lateral process of the talus is a rare injury, which is difficult to diagnose. As a result, early detection is often delayed, which in turn leads to ankle pain and dysfunction. We treated a patient by open reduction and screw fixation in fracture of the lateral process of talus and primary repair of the superior peroneal retinaculum. We report this case with a brief review of the literature.
- 543 View
- 0 Download

- Transscaphoidal Dorsal Perilunar Dislocation Associated with Dislocation of Distal Radioulnar Joint: A Case Report
- Chul Hyung Kang, Chul Hyun Cho, Dong Wan Kim
- J Korean Fract Soc 2014;27(1):77-81. Published online January 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.1.77
-
 Abstract
Abstract
 PDF
PDF - Dorsal perilunar dislocations are rare traumatic entities. Associated fractures such as carpal bones and radial styloid processes can occur. However, the dorsal perilunar dislocation associated with dislocation of distal radioulnar joint is extremely rare. The authors herein report the case of a 34-year-old man who was presented with transscaphoidal perilunar dislocation which is associated with dislocation of distal radioulnar joint.
- 414 View
- 0 Download

Original Article
- Intrapelvic Anterior Plate Fixation for Crescent Fracture-Dislocation of Sacroiliac Joint
- Kwang Jun Oh, Jin Ho Choi
- J Korean Fract Soc 2013;26(3):184-190. Published online July 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.3.184
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the radiological and clinical outcomes of intrapelvic anterior plate fixations for Day Classification Type II crescent fracture-dislocations of sacroiliac joints.
MATERIALS AND METHODS
Ten patients who had undertaken the surgical treatment for the sacroiliac joint from 2006 to 2012 were enrolled in this study. All cases fell into Type II by Day Classification for sacroiliac joint injuries. For surgical treatments, the plate fixation through the intra-pelvic anterior approach was first performed for all cases and anterior ring fixation was performed in 4 cases with more severely displaced anterior pelvic ring injuries. Then, radiological and clinical evaluation was implemented.
RESULTS
The bone union was observed from all patients whom performed the surgical fixation. In the radiological results, 9 cases with the anatomic and nearly-anatomic reductions were observed. Out of the 10 cases which performed the rotational displacement analysis, there were 3 excellent cases, 6 good cases and 1 fair case. The 10 cases that performed the deformity index and vertical displacement analysis, less variations were observed in the anterior ring fixations after intra-pelvic anterior plate fixation group. According to the clinical results, 4 excellent cases, 3 good cases, and 3 moderate cases were observed.
CONCLUSION
In the Type II crescent fracture-dislocation of sacroiliac joint, the intrapelvic anterior plate fixation achieved satisfactory anatomical reductions, radiological stabilities and clinical results.
- 580 View
- 6 Download

Case Reports
- Treatment of Traumatic Posterior Dislocation of the Sternoclavicular Joint: A Case Report
- Dong Hee Kim, Do Hoon Kim, Seok Kwon Kang, Eui Chul Lee
- J Korean Fract Soc 2013;26(1):56-59. Published online January 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.1.56
-
 Abstract
Abstract
 PDF
PDF - Compared with acromioclavicular dislocation, dislocation of the clavicle at its sternal end is uncommon and accounts for 3% of all injuries to the shoulder girdle. Furthermore, the posterior dislocation of the sternoclavicular joint is relatively a rare injury compared to the other types of sternoclavicular dislocation. We report this case since we have experience with similar cases of traumatic posterior dislocation at the sternoclavicular joint, which were successfully treated with x-ray guided reduction.
-
Citations
Citations to this article as recorded by- Posterior Sternoclavicular Dislocation: A Case Report
So Hwa Yoon, Sun Ki Kim, Ki Jun Kim
Journal of the Korean Society of Radiology.2015; 72(2): 128. CrossRef
- Posterior Sternoclavicular Dislocation: A Case Report
- 776 View
- 3 Download
- 1 Crossref

- Ipsilateral Distal Radius and Scaphoid Fractures Associated with Posteromedial Dislocation of the Elbow Joint: A Case Report
- Jin Wan Kim, Young Chul Ko, Chul Young Jung, Il Soo Eun, Young Jun Kim, Chang Kyu Kim
- J Korean Fract Soc 2012;25(2):150-154. Published online April 30, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.2.150
-
 Abstract
Abstract
 PDF
PDF - Arm injuries occurring from high energy injuries such as falls or traffic accidents can be accompanied by wrist and elbow injuries. Monteggia fracture, Galeazzi fracture, and Essex-Lopresti fracture-dislocation are known some examples of such injuries. However, there are no reports on the dislocation of the elbow occurring from a distal radius fracture accompanied by scaphoid fracture, and there is nothing published about its prognosis. The authors report on the treatment and outcomes of a case of a 42-year-old male who had a distal radius and scaphoid fracture associated with posteromedial dislocation of the elbow on the same side of his arm along with a literature review.
- 646 View
- 3 Download

- Combined Ipsilateral Fracture and Dislocation of Hip, Knee and Foot Joints: A Case Report
- Hyoung Soo Kim, Ju Hak Kim, Sang Joon Park, Jae Won Hyung
- J Korean Fract Soc 2012;25(1):73-76. Published online January 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.1.73
-
 Abstract
Abstract
 PDF
PDF - Although clinical cases of ipsilateral knee and hip joint dislocation have been reported, there are no reports of simultaneous ipsilateral hip, knee, and foot dislocations. We report here a case of a patient who had ipsilateral hip, knee, and foot joint dislocations, and review the relevant literature.
- 595 View
- 3 Download

Original Article
- Surgical Treatment of the Perilunate Dislocation and the Lunate Dislocation with Dorsal Approach
- Soo Hong Han, Jin Myoung Dan, Dong Hoon Lee, Young Woong Kim
- J Korean Fract Soc 2011;24(4):347-353. Published online October 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.4.347
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the clinical and radiologic outcomes of the perilunate dislocation and the lunate dislocation which were managed surgically through a dorsal approach.
MATERIALS AND METHODS
Retrospective reviews of the 13 patients who had minimum 1-year follow-up after surgical treatment through isolated dorsal approach for their perilunate dislocations or the lunate dislocations were performed. The case that dislocated lunate migrated proximally through the wrist was excluded in this series. We evaluated the DASH score in questionnaire method and Mayo wrist score to analyze the clinical outcomes. Radiologic results were investigated by measurement of the scapho-lunate angle, and fracture union was also evaluated in the case of trans-scaphoid dislocation.
RESULTS
The mean DASH Score was 16.3 points (range, 10.8~26.7 points) and the mean Mayo wrist score was 79 points (range, 65~90 points) at the final follow-up. There were 2 cases of excellent, 7 cases of good and 4 cases of fair in the Mayo wrist score. On the radiologic analysis, the mean scapho-lunate angle was 49.0degrees (range, 35~55degrees) and all cases were within the normal range. All cases of the trans-scaphoid perilunate dislocation achieved bone union.
CONCLUSION
Author's cases showed satisfactory outcomes in clinically and radiologically. Isolated dorsal approach could give anatomical reduction and appropriate internal fixation in treatment of the perilunate dislocations and the lunate dislocations except the rare case of proximal migration of the lunate through the wrist.
- 1,027 View
- 27 Download

Case Report
- Checkrein Deformity by Incarcerated Posterior Tibial Tendon and Displaced Flexor Hallucis Longus Tendon following Ankle Dislocation: A Case Report
- Su Young Bae, Hyung Jin Chung, Man Young Kim
- J Korean Fract Soc 2011;24(3):271-276. Published online July 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.3.271
-
 Abstract
Abstract
 PDF
PDF - We report a case of 20 year-old man who had unusual equinus and checkrein deformity following dislocation of his right ankle joint. He had been treated with distal tibiofibular screw fixation and external fixation. After removal of external fixator, he had suffered from progressive deformity of foot and ankle. Widening of distal tibiofibular joint and medial clear space was found on radiograph and it was revealed that posterior tibial tendon had been dislocated and incarcerated into the distal tibiofibular joint on MRI. We corrected the deformity with excision of incarcerated posterior tibial tendon, adhesiolysis and lengthening of flexor hallucis longus tendon, reconstruction of deltoid ligament and flexor digitorum longus tendon transfer.
-
Citations
Citations to this article as recorded by- Management of Checkrein Deformity
Min Gyu Kyung, Yun Jae Cho, Dong Yeon Lee
Clinics in Orthopedic Surgery.2024; 16(1): 1. CrossRef - A Neglected Extensor Hallucis Longus Tendon Rupture Caused by Arthritic Adhesion
Sung Hun Won, Sung Hwan Kim, Young Koo Lee, Dong-Il Chun, Byung-Ryul Lee, Woo-Jong Kim
Medicina.2023; 59(6): 1069. CrossRef - The Checkrein Deformity of Extensor Hallucis Longus Tendon and Extensor Retinaculum Syndrome with Deep Peroneal Nerve Entrapment after Triplane Fracture: A Case Report
Hyungon Gwak, Jungtae Ahn, Jae Hoon Lee
Journal of Korean Foot and Ankle Society.2021; 25(3): 145. CrossRef - Checkrein Deformity Due to Flexor Digitorum Longus Adhesion after Comminuted Calcaneus Fracture: A Case Report
Jin Su Kim, Han Sang Lee, Ki Won Young, Keun Woo Lee, Hun Ki Cho, Sang Young Lee
Journal of Korean Foot and Ankle Society.2015; 19(1): 35. CrossRef
- Management of Checkrein Deformity
- 743 View
- 0 Download
- 4 Crossref

Original Article
- Operative Treatment in the Delayed Diagnosed Fracture and Dislocation of Hamatometacarpal Joint
- Suk Ha Lee, Jong Wong Park, Jin Il Kim, Seoung Joon Lee
- J Korean Fract Soc 2011;24(3):249-255. Published online July 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.3.249
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose is to evaluate and report the results that treated with open reduction and internal fixation in delayed diagnosed fracture and dislocation of the hamatometacarpal joint.
MATERIALS AND METHODS
We evaluated 12 cases that had been treated with open reduction and internal fixation in delayed diagnosed fracture and dislocation of the hamatometacarpal joint. The mean interval between injury and operation was 34 days (21~60 days), the mean age of 12 cases was 28.1 years old, and mean follow-up period was 18 months. The computer tomography was done in all cases and the fracture and dislocation types were classified by Cain's classification. For the evaluation of results, pain scale, grasping power, range of motion of wrist and metacarpophalangeal joint were analyzed preoperatively and at final follow up, and the arthritic change of the hamatometacarpal joint was also checked.
RESULTS
According to Cain's classification, type Ia was one case, type Ib was two, type II was six, and type III was three. The pain scale was improved from 7.75 preoperatively to 0.92 at last follow up. The mean grasping power was improved up to 97.5% of normal. The preoperative range of motion of the wrist joint measured to be 60 degrees in extension and 70 degrees in flexion; the final range of motion indicated to be 75 degrees in extension and 80 degrees in flexion. The preoperative range of motion of the metacarpophalangeal joint measured to be 0 degrees in extension and 70 degrees in flexion; the final range of motion indicated to be 0 degrees in extension and 85 degrees in flexion. Carpometacarpal arthritis was developed in two cases.
CONCLUSION
The open reduction and internal fixation is considered as one of good treatment option in the delayed diagnosed hamatometacarpal fracture and dislocation. -
Citations
Citations to this article as recorded by- Reliability of classification of ring and little finger carpometacarpal joint fracture subluxations: a comparison between two-dimensional computed tomography and three-dimensional computed tomography classifications
J. H. Kim, S.-S. Kwon, S. J. Moon, J. S. Choe, H. I. Kwak, S. Y. Lee, H. J. Le, J. Y. Kim
Journal of Hand Surgery (European Volume).2016; 41(4): 448. CrossRef - Fourth and Fifth Metacarpal Base Arthrodesis for Posttraumatic Arthritis of Fifth Carpometacarpal Joint
Chul-Hyung Kang, Eun-Sok Son, Chul-Hyun Cho
Journal of the Korean Society for Surgery of the Hand.2013; 18(4): 184. CrossRef
- Reliability of classification of ring and little finger carpometacarpal joint fracture subluxations: a comparison between two-dimensional computed tomography and three-dimensional computed tomography classifications
- 809 View
- 1 Download
- 2 Crossref

Case Reports
- Bilateral Open Transcalcaneal Fracture with Talonavicular Dislocation: A Case Report
- Hun Park, Sung Jin Shin, Sang Rim Kim, Kwang Woo Nam, Sung Wook Choi, Kyu Bum Seo, Jun Young Seo
- J Korean Fract Soc 2011;24(1):87-91. Published online January 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.1.87
-
 Abstract
Abstract
 PDF
PDF - Although calcaneal fracture is relatively common in ankle injury, open intraarticular calcaneal fracture with dorsal dislocation of the navicular from talus is extremely rare and severe injury. There are few data which are available concerning the injury mechanism and treatment options. The purpose of this report is to describe a case with bilateral open transcalcaneal fracture with talonavicular dislocation and to discuss the prevalence, mechanism of this injury, and treatment options.
-
Citations
Citations to this article as recorded by- Results in Operative Treatment of Open Calcaneal Fracture
Ba Rom Kim, Jun Young Lee, Donghyuk Cha
Journal of Korean Foot and Ankle Society.2021; 25(3): 133. CrossRef
- Results in Operative Treatment of Open Calcaneal Fracture
- 694 View
- 2 Download
- 1 Crossref

- Dislocation of the Shoulder with Ipsilateral Humeral Shaft Fracture: A Case Report
- Chul Hyun Cho, Kwang Yeung Jeong
- J Korean Fract Soc 2010;23(4):382-385. Published online October 31, 2010
- DOI: https://doi.org/10.12671/jkfs.2010.23.4.382
-
 Abstract
Abstract
 PDF
PDF - Dislocation of the shoulder with ipsilateral humeral shaft fracture is very rare, but serious injury that requires emergent care. There have been approximately 20 cases reported in the English literature, but it has never been reported in Korea. We report a case of dislocation of right shoulder with ipsilateral humeral shaft fracture which was successfully treated by closed reduction of the shoulder under general anesthesia and internal fixation with antegrade interlocking intramedullary nailing for the humeral shaft fracture.
-
Citations
Citations to this article as recorded by- Anterior Shoulder Dislocation With an Ipsilateral Humeral Shaft Fracture: A Case Report
Abdulmalik B Albaker , Ahmad Abdullah A Alsaleh, Mishari Malik Alshammari, Hatim Abdullah Akkasi, Hazzaa Abdullah Hazza Alharbi, Norah Ibrahim S Alqurmulah
Cureus.2023;[Epub] CrossRef
- Anterior Shoulder Dislocation With an Ipsilateral Humeral Shaft Fracture: A Case Report
- 829 View
- 1 Download
- 1 Crossref

Original Article
- Arthroscopic Treatment of Acromioclavicular Joint Dislocation Using TightRope(R): Preliminary Report
- Eui Sung Choi, Kyoung Jin Park, Yong Min Kim, Dong Soo Kim, Hyun Chul Shon, Byung Ki Cho, Ji Kang Park, Hyun Chul Lee
- J Korean Fract Soc 2010;23(3):310-316. Published online July 31, 2010
- DOI: https://doi.org/10.12671/jkfs.2010.23.3.310
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the clinical and radiologic results of the arthroscopic treatment using TightRope(R) (Arthrex, Inc, Naples, FL) for management of acute acromioclavicular dislocation.
MATERIALS AND METHODS
Twelve patients with acromioclavicular joint dislocation Rockwood type V are underwent the arthroscopic acromioclavicular joint reconstruction using TightRope(R) between March, 2008 and March, 2009. The average age was 40.4 years (range 25~63 years) and mean follow-up was 10 months (range 8~16 months). The shoulders were evaluated using parameters include radiologic measurements by comparing the clavicle posteroanterior and lateral radiographs with the contralateral one. Clinical evaluation was made for pain, function, and range of joint motion by Constant score and KSS (Korean Shoulder Score).
RESULTS
All twelve patients returned to their work without pain in 3 months after operation. The average Constant score and KSS score was 98.4 (range 97~100) and 97.8 (range 97~100) at the last follow-up. Because of technical error and indication error, two patients showed failures of TightRope(R) fixation on the coracoid side and the acromioclavicular joint was redislocated, so these cases were excluded. 10 patients were satisfied with functional results and cosmetic appearance.
CONCLUSION
Considering its less morbidity, less hospitalization, excellent cosmesis, early rehabilitation, this new technique offers an attractive alternative in acromioclavicular joint stabilization if the early technical error would be overcome. -
Citations
Citations to this article as recorded by- Coracoclavicular Ligament Augmentation Using Tight-Rope®for Acute Acromioclavicular Joint Dislocation - Preliminary Report -
Seok Hyun Kweon, Sang Su Choi, Seong In Lee, Jeong Woo Kim, Kwang Mee Kim
The Journal of the Korean Shoulder and Elbow Society.2013; 16(2): 115. CrossRef - Coracoclavicular Ligament Augmentation Using Endobutton for Unstable Distal Clavicle Fractures - Preliminary Report -
Chul-Hyun Cho, Gu-Hee Jung, Hong-Kwan Sin, Young-Kuk Lee, Jin-Hyun Park
The Journal of the Korean Shoulder and Elbow Society.2011; 14(1): 1. CrossRef
- Coracoclavicular Ligament Augmentation Using Tight-Rope®for Acute Acromioclavicular Joint Dislocation - Preliminary Report -
- 753 View
- 5 Download
- 2 Crossref

Case Reports
- Fracture-Dislocation of S1 in 3-Year-Old Boy: A Case Report
- Sang Bong Ko, Sang Wook Lee
- J Korean Fract Soc 2010;23(2):232-235. Published online April 30, 2010
- DOI: https://doi.org/10.12671/jkfs.2010.23.2.232
-
 Abstract
Abstract
 PDF
PDF - Fracture-dislocation of the sacrum that has not yet fully developed is common in the distal sacrococcygeal joint of children, but this injury is rarely seen in 1st Sacrum. Most of these patients have a severe neurological deficit, so this injury generally requires surgical decompression. We managed a three year old patient who had a S1 fracture-dislocation without a neurological deficit, and the patient was treated with simple skin traction and bed rest without surgery. The child had a satisfactory result, so we report on this case with reviewing the relevant literatures.
- 452 View
- 1 Download

- Posterior Hip Dislocation with Ipsilateral Fractures of the Femoral Head and Intertrochanter: A Case Report
- Jai Hyung Park, Hyung Soo Kim, Soo Tae Chung, eong Hyun Yoo, Joo Hak Kim, Seung Do Cha, Tae Woo Lee
- J Korean Fract Soc 2010;23(1):113-117. Published online January 31, 2010
- DOI: https://doi.org/10.12671/jkfs.2010.23.1.113
-
 Abstract
Abstract
 PDF
PDF - High-energy injury, as traffic accident or fall down, can cause fracture of femur head and posterior dislocation of hip joint which is accompanied with ipsilateral acetabulum fracture or femur neck fracture. But the case that femur head fracture and posterior dislocation of the hip joint coincide with ipsilateral intertrochanteric fracture of proximal femur is so uncommon that reports of the case is very rare. We hereby are to report the experienced and treated-cases of femur head fracture and posterior dislocation of the hip joint that is accompanied with ipsilateral intertrochanteric fracture.
-
Citations
Citations to this article as recorded by- Decoding the behaviour of extracapsular proximal femur fracture- dislocation - A systematic review of a rare fracture pattern
Keyur B. Desai
Journal of Clinical Orthopaedics and Trauma.2021; 18: 157. CrossRef
- Decoding the behaviour of extracapsular proximal femur fracture- dislocation - A systematic review of a rare fracture pattern
- 734 View
- 3 Download
- 1 Crossref

- Clavicle Midshaft Fracture with Acromioclavicular Joint Dislocation: A Case Report
- Chul Hyun Cho, Chul Hyung Kang, Soo Won Jung, Hyuk Jun Seo
- J Korean Fract Soc 2009;22(4):297-299. Published online October 31, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.4.297
-
 Abstract
Abstract
 PDF
PDF - Clavicle fracture or acromioclavicular joint dislocation is common injury in the upper extremity. But ipsilateral clavicle midshaft fracture with acromioclavicular joint dislocation is a extremely rare. Seven cases has been reported in the English literature, but it has never been reported in Korea. We report a case of clavicle midshaft fracture with acromioclavicular joint dislocation caused by motor vehicle accident and describe its presumed mechanism, diagnosis, treatment with a review of literature.
- 565 View
- 6 Download

- Bilateral Malunion and Distal Radioulnar Joint Dislocation after Operative Treatment of Bilateral Galeazzi Fractures in Child: A Case Report
- Sang Jin Cheon, Dong Joon Kang, Nam Hoon Moon, Seung Han Cha, He Myung Cho
- J Korean Fract Soc 2009;22(4):292-296. Published online October 31, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.4.292
-
 Abstract
Abstract
 PDF
PDF - Galeazzi fractures in child is rare and seldom necessary of operative treatment because the result of conservative treatment is good. We present the patient who was a 11-year-old male and fell onto his both hands during a hundred-meter dash. His diagnosis was bilateral Galeazzi fractures and limited open reduction and internal fixation with Kirschner pins was initial treatment at local hospital. After 4 weeks postoperatively, Kirschner pins were removed and rehabilitating exercise was started. After 4 months postoperatively, he was transferred to our hospital due to malunion with severe angular deformities and distal radioulnar joint (DRUJ) dislocation. He was treated with corrective osteotomy. Thus, as in this case, we suggest more careful treatment and observation if conservative method of Galeazzi fracture in child is chosen and consider operative method as treatment according to age and pattern of fracture.
- 681 View
- 1 Download

Original Article
- Long Term Follow up Results of the Operative Treatment of the Acromioclavicular Joint Dislocation with a Wolter Plate
- Ki Ser Kang, Han Jun Lee, Jae Sung Lee, Jae Yoon Kim, Yong Beom Park
- J Korean Fract Soc 2009;22(4):259-263. Published online October 31, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.4.259
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the long-term clinical and radiological results of the operative treatment of the acromioclavicular dislocation with a Wolter plate. MATERIALS AND METHODS: We reviewed clinical and radiological data of twenty patients (mean age: 37 years) who underwent the operative treatment of acromioclavicular joint dislocation using a Wolter plate from September, 1999 to December, 2002 with minimum of five years follow-up (average 6 years 7 months). The clinical outcomes of twenty patients were evaluated by UCLA scoring and radiological results of fifteen patients with available radiograph were evaluated by Zanca view and stress view. RESULTS: The mean UCLA score was mean 33 points (range, 27~35) at final follow up. By clinical evaluation, twelve cases (60%) were excellent, six cases (30%) were good and two cases were poor (10%). By radiological evaluation, eight cases (54%) were excellent (without displacement), five cases (33%) were good (displacement <5 mm) and two cases (13%) were poor (displacement >5 mm). Erosive change in acromioclavicular joint was seen in poor case. CONCLUSION: Wolter plate fixation may be a useful modality for treating acromioclavicular joint dislocation. Great care should be taken to make the hook hole at the appropriate position during operation for long-term prognosis. -
Citations
Citations to this article as recorded by- Clinical outcomes of bending versus non-bending of the plate hook in acromioclavicular joint dislocation
Min Su Joo, Hoi Young Kwon, Jeong Woo Kim
Clinics in Shoulder and Elbow.2021; 24(4): 202. CrossRef - Clinical Comparison of Two Types of Hook Plate in Surgical Treatment of Acromioclavicular Dislocation - AO Hook Plate and Wolter Plate -
Jea-Yeol Choi, Eugene Kim, Haw-Jae Jeong, Jin Whan Ahn, Hun-Kyu Shin, Se-Jin Park, Seung-Hee Lee, Jae-Wook Lee, Kyu-Bo Choi
The Journal of the Korean Shoulder and Elbow Society.2012; 15(2): 123. CrossRef
- Clinical outcomes of bending versus non-bending of the plate hook in acromioclavicular joint dislocation
- 751 View
- 2 Download
- 2 Crossref

Case Report
- Patient Accompanied with Simultaneous Anterior Dislocation of Hip and Anterior Dislocation of Knee : A Case Report
- Hee Gon Park
- J Korean Fract Soc 2009;22(3):185-188. Published online July 31, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.3.185
-
 Abstract
Abstract
 PDF
PDF - We are reporting a case that a 61-year-old patient who had simultaneous anterior dislocation of left hip and anterior dislocation of right knee after fall from a height injury was treated by closed reduction respectively.
-
Citations
Citations to this article as recorded by- Combined Ipsilateral Fracture and Dislocation of Hip, Knee and Foot Joints - A Case Report -
Hyoung-Soo Kim, Ju-Hak Kim, Sang-Joon Park, Jae-Won Hyung
Journal of the Korean Fracture Society.2012; 25(1): 73. CrossRef
- Combined Ipsilateral Fracture and Dislocation of Hip, Knee and Foot Joints - A Case Report -
- 676 View
- 1 Download
- 1 Crossref

Original Article
- Crescent Fracture-dislocation of Sacroiliac Joint: Affecting Factors of Operative Results
- Hee Soo Kim, Chang Wug Oh, Poong Taek Kim, Young Soo Byun, Joo Woo Kim, Byung Chul Park, Woo Kie Min, Hyun Joo Lee
- J Korean Fract Soc 2009;22(2):71-78. Published online April 30, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.2.71
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To assess the affecting factors of results after the operation of Crescent fracture-dislocation in sacro-iliac joint.
MATERIALS AND METHODS
In 19 patients (mean age, 47.4 year-old) of open reduction and internal fixation for Crescent fracture-dislocation, there were seven type I, 9 type II, and 3 type III fractures according to Day's classification. We assessed affecting factors of radiological and functional results, such as patients' ages, surgical approaches, the fixation extent of pelvic ring, and fracture patterns.
RESULTS
Seventeen of 19 cases united at 14.5 weeks in average, and 2 non-unions occurred with the fixation failure of posterior ring. Satisfactory results were 14 and 15 in radiological and functional evaluation, respectively. In complications, three cases of leg length discrepancy were from an imperfect reduction and two fixation failures. Surgical approach did not show any difference of results, but all cases of unsatisfactory reduction occurred from posterior ring fixation through the anterior approach. Fixation of both rings seemed to have satisfactory results, comparing to posterior ring only. Older patients over 60 year-old had more complications and a tendency to show an unsatisfactory result.
CONCLUSION
In operative treatment of Crescent fracture-dislocation of sacro-iliac joint, it is better to fix both anterior and posterior rings. But, caution is needed to prevent complications in old-aged patients. -
Citations
Citations to this article as recorded by
- 1,376 View
- 52 Download
- 2 Crossref

Case Reports
- Irreducible Dislocation of the Interphalangeal Joint of the Great Toe with Lateral Collateral Ligament Entrapment: A Case Report
- Duke Whan Chung, Bi O Jeong
- J Korean Fract Soc 2009;22(2):110-113. Published online April 30, 2009
- DOI: https://doi.org/10.12671/jkfs.2009.22.2.110
-
 Abstract
Abstract
 PDF
PDF - Dislocations of the interphalangeal joint of the great toe that are irreducible are very rare. Invagination of the plantar plate or the sesamoid bone into the IP joint, which prevents reduction. To our knowledge, however, dislocations of the IP joint of the great toe that were irreducible because of lateral collateral ligament entrapment, not invagination of the plantar plate or the sesamoid bone, have not been reported by any English literature. We report a 29-year-old ballet dancer who sustained an irreducible dislocation of the interphalangeal joint of the great toe owing to lateral collateral ligament entrapment.
-
Citations
Citations to this article as recorded by- Open Reduction of a Dislocation of the Interphalangeal Joint of the Great Toe Neglected for 6 Weeks
Jae Kwang Kim, Rag-Gyu Kim
Journal of the Korean Orthopaedic Association.2011; 46(5): 426. CrossRef
- Open Reduction of a Dislocation of the Interphalangeal Joint of the Great Toe Neglected for 6 Weeks
- 1,180 View
- 4 Download
- 1 Crossref

- Bipolar Clavicular Dislocation: A Case Report
- Han Jun Lee, Jae Sung Lee, Young Bong Ko
- J Korean Fract Soc 2008;21(4):316-319. Published online October 31, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.4.316
-
 Abstract
Abstract
 PDF
PDF - Bipolar clavicular dislocation is simultaneous dislocation of both poles of the clavicle (mainly an anterior dislocation of the sternoclavicular joint and a posterior dislocation of acromioclavicular joint) and rarely reported. We report a case of bipolar claviclular dislocation after a seat belt injury and describe its presumed mechanism and treatment with a review of literature.
-
Citations
Citations to this article as recorded by- Case of the Month #177: Bipolar Clavicular Dislocation: Radiologic Evaluation of a Rare Traumatic Injury
Michael P. Loreto, Dawn Pearce
Canadian Association of Radiologists Journal.2012; 63(2): 156. CrossRef - Clavicle Midshaft Fracture with Acromioclavicular Joint Dislocation: A Case Report
Chul-Hyun Cho, Chul-Hyung Kang, Soo-Won Jung, Hyuk-Jun Seo
Journal of the Korean Fracture Society.2009; 22(4): 297. CrossRef
- Case of the Month #177: Bipolar Clavicular Dislocation: Radiologic Evaluation of a Rare Traumatic Injury
- 759 View
- 3 Download
- 2 Crossref

- Lateral Dislocation of the First Metatarsophalangeal Joint: A Case Report
- Yeong Sik Yun, Young Mo Kim, Kyung Cheon Kim, Pil Sung Kim
- J Korean Fract Soc 2008;21(4):312-315. Published online October 31, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.4.312
-
 Abstract
Abstract
 PDF
PDF - Dislocation of the metatarsophalangeal joint is rare due to the stability of the ligaments and soft tissue surrounding the joint. The authors have experienced lateral dislocation of the first metatarsophalangeal joint, which required surgery, accompanied by complete injuries of medial collateral ligament and capsule, contributing to medial stability, differing from posterior dislocation with intersesamoid complex rupture, with a review of the relevant literature and previous reported cases.
-
Citations
Citations to this article as recorded by- An Unusual Combination of Injuries Involving Lateral Dislocation of the First and Fifth Metatarsophalangeal Joints Along With Fractures of the Other Toes on the Same Foot: A Report of a Rare Case
Mohamed Jiddi, Georges F Bassil, Zied Missaoui
Cureus.2025;[Epub] CrossRef - Dislocation of the first metatarsophalangeal joint concomitant with Lisfranc joint dislocation in a 45-year-old man
Kanoko Mizumoto, Tadashi Kimura, Makoto Kubota, Mitsuru Saito
BMJ Case Reports.2021; 14(6): e243004. CrossRef - Rare Lateral Dislocation of the First Metatarsophalangeal Joint: A Case Report and Review of the Literature
Amir Reza Vosoughi, Pascal F. Rippstein
The Journal of Foot and Ankle Surgery.2017; 56(2): 375. CrossRef
- An Unusual Combination of Injuries Involving Lateral Dislocation of the First and Fifth Metatarsophalangeal Joints Along With Fractures of the Other Toes on the Same Foot: A Report of a Rare Case
- 965 View
- 5 Download
- 3 Crossref

Original Article
- Fracture-Dislocation of the Carpometacarpal Joint with the Fracture of Hamate
- Jin Woong Yi, Whan Young Chung, Woo Suk Lee, Cheol Yong Park, Youn Moo Heo
- J Korean Fract Soc 2008;21(4):297-303. Published online October 31, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.4.297
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the classification and treatment results about the injury of carpometacarpal (CMC) joint with the fracture of hamate.
MATERIALS AND METHODS
The authors categorized into 3 types (I, II, III) according to the location of injured CMC joint and type II was subdivided into 2 type (a, b) according to the size of coronal fragment of hamate fracture-type I: fracture-dislocation of 5th CMC joint with small-sized fragment or avulsion fracture of hamate, type IIa: fracture-dislocation of 4th and 5th CMC joint with small-sized fragment or avulsion fracture of hamate, type IIb: fracture-dislocation of 4th and 5th CMC joint with coronal fracture of hamate body presenting an oblique or coronal splitting fracture, and type III: type II injury associated with injury of 3rd CMC joint or coronal plane fracture of capitate. All cases were carried out the operative treatment. And radiologic results and clinical results were evaluated.
RESULTS
Type I were 2 cases, type IIa 4, type IIb 5, and type III 3. Twelve of 14 cases were excellent or good results, 1 case (type III) was fair, and 1 case (type IIa) was poor. All cases obtained anatomic reduction of CMC joint. But, the posttraumatic arthritis was observed in 1 case (poor) and the displacement of non-fixed hamate fragment was observed in 1 case (fair).
CONCLUSION
We think that it may get more favorable outcomes by the fixation of the relative large fragment of hamate with anatomical reduction of CMC joint. -
Citations
Citations to this article as recorded by- Operative treatment of hamate fractures with hamatometacarpal fracture dislocation using a self-designed dorsal buttress locking plate with trans-metacarpal pin insertion: short-term follow-up results
Seok-Won Kim, Hyung-Joon Lee, Ji-Kang Park, Dong-Min Chung
Archives of Hand and Microsurgery.2022; 27(3): 193. CrossRef - Operative Treatment of Trapezium Fractures
Ho Jung Kang, Nam Heon Seol, Man Seung Heo, Soo-Bong Hahn
Journal of the Korean Fracture Society.2009; 22(4): 276. CrossRef
- Operative treatment of hamate fractures with hamatometacarpal fracture dislocation using a self-designed dorsal buttress locking plate with trans-metacarpal pin insertion: short-term follow-up results
- 952 View
- 3 Download
- 2 Crossref

Case Reports
- Irreducible Dislocation of the Interphalangeal Joint of the Thumb: A Case Report
- Phil Hyun Chung, Suk Kang, Chung Soo Hwang, Jong Pil Kim, Young Sung Kim, Kwang Uk An
- J Korean Fract Soc 2008;21(2):165-168. Published online April 30, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.2.165
-
 Abstract
Abstract
 PDF
PDF - Dislocations of the interphalangeal joint of the thumb are rather uncommon as a result of the inherent stability of the interphalangeal joint. Irreducible dislocations of these joint are rare. The authors report a case of irreducible dislocation of the interphalangeal joint of the thumb with interposed palmar plate, and reduced by open reduction.
- 812 View
- 27 Download

- Anterior Dislocation of Distal Radio-Ulnar Joint: A Case Report
- Shin Kun Kim, Sang Bong Ko, Seung Bum Chae
- J Korean Fract Soc 2008;21(1):66-69. Published online January 31, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.1.66
-
 Abstract
Abstract
 PDF
PDF - There are variable types in wrist joint injury. Most common case is simple distal radius fracture. And ulnar head dislocation associated with disruption of distal radioulnar ligament is unusual. Among thease injury types. volar dislocation of ulnar head in the distal radioulnar joint is not common and it is misdiagnosis frequently. So it needs to surgical operation frequently. The author reviews this injury with the relevant literature.
- 634 View
- 6 Download

- Traumatic Bilateral Anterior Hip Dislocation: A Case Report
- Sung Taek Jung, Hyun Jong Kim, Myung Sun Kim, Young Jin Kim, Sang Kwan Cho
- J Korean Fract Soc 2008;21(1):62-65. Published online January 31, 2008
- DOI: https://doi.org/10.12671/jkfs.2008.21.1.62
-
 Abstract
Abstract
 PDF
PDF - Traumatic anterior dislocation of the hip is an uncommon injury, accounting for less than 10% of all reported cases of traumatic hip dislocation. Especially, there are no known report in our country so far. We are reporting a case of a 81 year old man who sustained bilateral anterior hip dislocation after pedestrian traffic accident, and treated by closed reduction and skeletal traction at our institute.
- 440 View
- 2 Download

- Traumatic Simultaneous Bilateral Hip Dislocation in the Elderly Patient: A Case Report
- Koing Woo Keon, Sang Bong Ko
- J Korean Fract Soc 2007;20(4):335-338. Published online October 31, 2007
- DOI: https://doi.org/10.12671/jkfs.2007.20.4.335
-
 Abstract
Abstract
 PDF
PDF - Traumatic simultaneous bilateral hip dislocation is reported rarely, but the most of them are limited in young patients. The authors managed the elderly patients whose both hip was dislocated traumatically, simultaneously and who didn't have any other underlying disease and other associated fracture - femur, hip joint and pelvis, with a review of the relevant literature.
- 471 View
- 1 Download

- Vertically Unstable Fracture of the Pelvis Combined with Anterior Dislocation of the Hip Joint: A Case Report
- Kap Jung Kim, Ha Yong Kim, Dae Suk Yang, Won Sik Choy
- J Korean Fract Soc 2007;20(3):272-276. Published online July 31, 2007
- DOI: https://doi.org/10.12671/jkfs.2007.20.3.272
-
 Abstract
Abstract
 PDF
PDF - Pelvic fractures result from high energy trauma and often associated with concomitant injuries. But, vertically unstable pelvic fractures combined with anterior dislocation of the hip is far less common. The traumatic dislocation of the hip is a true orthopedic emergency and it should be considered that a femoral head can be exposed to deteriorized vascularity. We report a case of vertically unstable pelvic fractures combined with traumatic anterior dislocation of the hip joint with the review of the literature.
- 549 View
- 1 Download

- Hip Fracture-dislocation with Sciatic Nerve Palsy and Ipsilateral Femoral Shaft Open Fracture: A Case Report
- Kap Jung Kim, Ha Yong Kim, Sung Il Kang, Won Sik Choy
- J Korean Fract Soc 2007;20(1):94-98. Published online January 31, 2007
- DOI: https://doi.org/10.12671/jkfs.2007.20.1.94
-
 Abstract
Abstract
 PDF
PDF - The posterior dislocation of the hip accounts for about 85~90% of traumatic hip dislocations and high energy mechanisms such as traffic accidents may cause them. The traumatic dislocation and fracture-dislocation of the hip are true orthopedic emergencies and it should be considered that a femoral head has poor vascularity and the sciatic nerve is closely located to it. We report on one patient who went through the surgical treatment of the concomitant ipsilateral open fracture of the femoral shaft and hip fracture-dislocation accompanying sciatic nerve injury with the review of the literatures.
- 764 View
- 4 Download

Original Article
- Modified Phemister Technique with Tension Band Wiring in Acromioclaviculr Joint Dislocation
- Yu Jin Kim, Hun Kyu Shin, Ji Won Lee
- J Korean Fract Soc 2006;19(4):431-436. Published online October 31, 2006
- DOI: https://doi.org/10.12671/jkfs.2006.19.4.431
-
 Abstract
Abstract
- PURPOSE
To evaluate the clinical and radiological result of surgical treatment of acromioclavicular joint dislocation, using modified Phemister technique with tension band wiring.
MATERIALS AND METHODS
We chose 17 patients who were able to follow up 1 year or more among the patients who were diagnosed as acromioclavicular joint dislocation in our hospital through January 2000 to Feburary 2005 and took modified Phemister technique with tension band wiring. Evaluation of the surgical results was done with the condition of pain, activity of daily living, range of motion, muscle tone by constant score system, and with preoperative, postoperative and last follow up radiographs.
RESULTS
Clinical evaluation was average 92 point by Constant score system from 84 point to 100 point. Subjective evaluation was 11 excellent (65%), 6 good (35%). Radiological evaluation was 9 excellent (54%), 6 good (38%), 2 fair (12%), and no poor group. On the final follow up, two cases showed inflammatory reaction at where pins were inserted, but after the removal of the pins, the inflammation was subsided.
CONCLUSION
The modified Phemister surgery for acromioclavicular dislocation is one of effective techniques, we can obtain firm fixation, exercise full range of motion early and there is no complication of re-dislocation.
- 527 View
- 0 Download

Case Report
- Simultaneous Dorsal Dislocation of Interphalangeal Joints in the Same Finger: Two Case Report
- Hyun Seok Song, Suk Ku Han, Sung Jin Park, Won Sik Nam, Hyuk Jae Yang, Nam Yong Choi
- J Korean Fract Soc 2006;19(3):388-391. Published online July 31, 2006
- DOI: https://doi.org/10.12671/jkfs.2006.19.3.388
-
 Abstract
Abstract
- We treated 2 cases of simultaneous dorsal dislocation of interphalangeal joints in the 5th finger. One case was injured by herperextension during basketball, and treated by open reduction and K-wire fixation. Another case was injured by industrial accident, and treated by splint for 1 week.
-
Citations
Citations to this article as recorded by- Double Dislocation of Interphalangeal Joints in a Single Digit - A Case Report -
Jai Hyung Park, Jeong Hyun Yoo, Joo Hak Kim, In Hyeok Lee
Journal of the Korean Society for Surgery of the Hand.2012; 17(4): 196. CrossRef
- Double Dislocation of Interphalangeal Joints in a Single Digit - A Case Report -
- 644 View
- 0 Download
- 1 Crossref

Original Article
- Clinical and Functional Result after Internal Fixation of Severely Displaced Floating Shoulder
- Sang Hun Ko, Chang Hyuk Choe, Sung Do Cho, Jae Sung Seo, Jong Oh Kim, Jaedu Yu, Sang Jin Shin, In Ho Jeon, Kwang Hwan Jung, Jong Keun Woo, Ji Young Jeong, Gwon Jae No
- J Korean Fract Soc 2006;19(1):46-50. Published online January 31, 2006
- DOI: https://doi.org/10.12671/jkfs.2006.19.1.46
-
 Abstract
Abstract
- PURPOSE
To evaluate the follow-up result of 11 cases that were operated with internal fixation of scapular neck and internal fixation of clavicle or acromioclavicular dislocation for severely displaced floating shoulder which was high energy injury and unstable.
MATERIALS AND METHODS
We examined the scapular neck fracture with clavicle fracture or acromioclavicular joint dislocation by multidisciplinary research from August 1997 to July 2004. The scapular neck fractures were operated in the case of translational displacement of more than 25 mm and angular displacement of more than 45 degrees with 3.5 mm reconstruction plate fixation and internal fixation for clavicle fracture or acromioclavicular joint perpormed simultaneously. And we evaluated 11 cases that can be followed up for more than 9 months.
RESULTS
We achieved bony union in all cases. In ASES functional score, we got average 89.2 (75~95) points. In Rowe functional score, we got average 89.1 (75~100) points. In complication, there was external rotation weakness in 1 case.
CONCLUSION
In severely displaced floating shoulder due to high energy injury, we got good clinical and functional result after internal fixation for scapular neck and clavicle or acromioclavicular joint.
- 401 View
- 0 Download


 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS

 First
First Prev
Prev


