Articles
- Page Path
- HOME > J Musculoskelet Trauma > Volume 39(2); 2026 > Article
-
Review Article
- Combined acetabular and pelvic ring injuries: a reference-frame algorithm for definitive fixation sequencing
-
Jeong-Hyun Koh
 , Seungyeob Sakong
, Seungyeob Sakong
-
Journal of Musculoskeletal Trauma 2026;39(2):83-92.
DOI: https://doi.org/10.12671/jmt.2026.00031
Published online: March 31, 2026
Department of Orthopedic Surgery, Ajou University School of Medicine, Suwon, Korea
- Correspondence to: Seungyeob Sakong Department of Orthopedic Surgery, Ajou University School of Medicine, 164 Worldcup-ro, Yeongtong-gu, Suwon 16499, Korea Tel: +82-31-219-5220, Email: sgsy4040@gmail.com
© 2026 The Korean Orthopaedic Trauma Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 409 Views
- 15 Download
- Abstract
- Introduction
- Scope, terminology, and classification
- Working framework: MCAPI vs. non-MCAPI
- Epidemiology, injury patterns, and assessment pearls for definitive planning
- Decision points and operative planning
- Definitive fixation strategy and sequence
- Outcomes, complications, and postoperative considerations
- Discussion: pitfalls, controversies, and future directions
- Summary and key messages
- Article Information
- References
Abstract
- Combined acetabular and pelvic ring injuries are not simply “two fractures in one patient.” Reduction and fixation of one component can alter the alignment and reducibility of the other, rendering operative sequencing a primary decision variable rather than a secondary consideration. These injuries typically result from high-energy trauma, frequently occur in patients with polytrauma, and are further influenced by physiological tolerance and the feasibility of available operative corridors. The existing evidence base remains constrained by retrospective study designs, inconsistent definitions, variable classification systems, and heterogeneous outcome reporting, all of which limit the strength of comparative recommendations. This state-of-the-art review presents a surgeon-facing, algorithmic approach grounded in a reference-frame mindset. We emphasize computed tomography (CT)-based mapping and the use of consistent terminology to characterize acetabular morphology, pelvic ring instability, deformity vectors, suspicion of mechanical coupling, and feasible operative corridors. Mechanically connected acetabular and pelvic ring injuries (MCAPI) are introduced as a working framework for identifying patterns in which reduction or fixation of one injury predictably influences the other. In cases of suspected MCAPI, a posterior ring-based sequence is generally preferred, typically consisting of posterior ring reduction and fixation, definitive acetabular reconstruction, and subsequent anterior ring fixation. We propose an explicit intraoperative “GO/NO-GO” checkpoint (reference acceptable, stable, corridors feasible) to prevent acetabular reconstruction on a moving target. Acetabulum-first strategies may be appropriate only in selected anteroposterior compression-type configurations in which acetabular fixation plausibly restores sacroiliac congruency and posterior stabilization remains technically feasible. We summarize key outcome domains and complication patterns, highlighting hip dislocation as an important risk factor associated with both neurologic deficits and overall complications. Standardized CT-based definitions and outcome instruments, together with multicenter cohorts employing predefined decision pathways, are required to test sequencing strategies and to determine whether improved radiographic reduction translates into durable functional benefit.
Introduction
Scope, terminology, and classification
Working framework: MCAPI vs. non-MCAPI
Epidemiology, injury patterns, and assessment pearls for definitive planning
Decision points and operative planning
Definitive fixation strategy and sequence
Outcomes, complications, and postoperative considerations
Discussion: pitfalls, controversies, and future directions
Summary and key messages
-
Author contributions
Conceptualization: JHK, SS. Methodology: JHK, SS. Investigation: JHK. Resources: JHK. Data curation: JHK. Supervision: SS. Project administration: SS. Visualization: JHK. Writing–original draft: JHK. Writing–review & editing: JHK. SS. All authors read and approved the final manuscript.
-
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
-
Funding
None.
-
Data availability
Not applicable.
-
Acknowledgments
None.
-
Supplementary materials
None.
Article Information
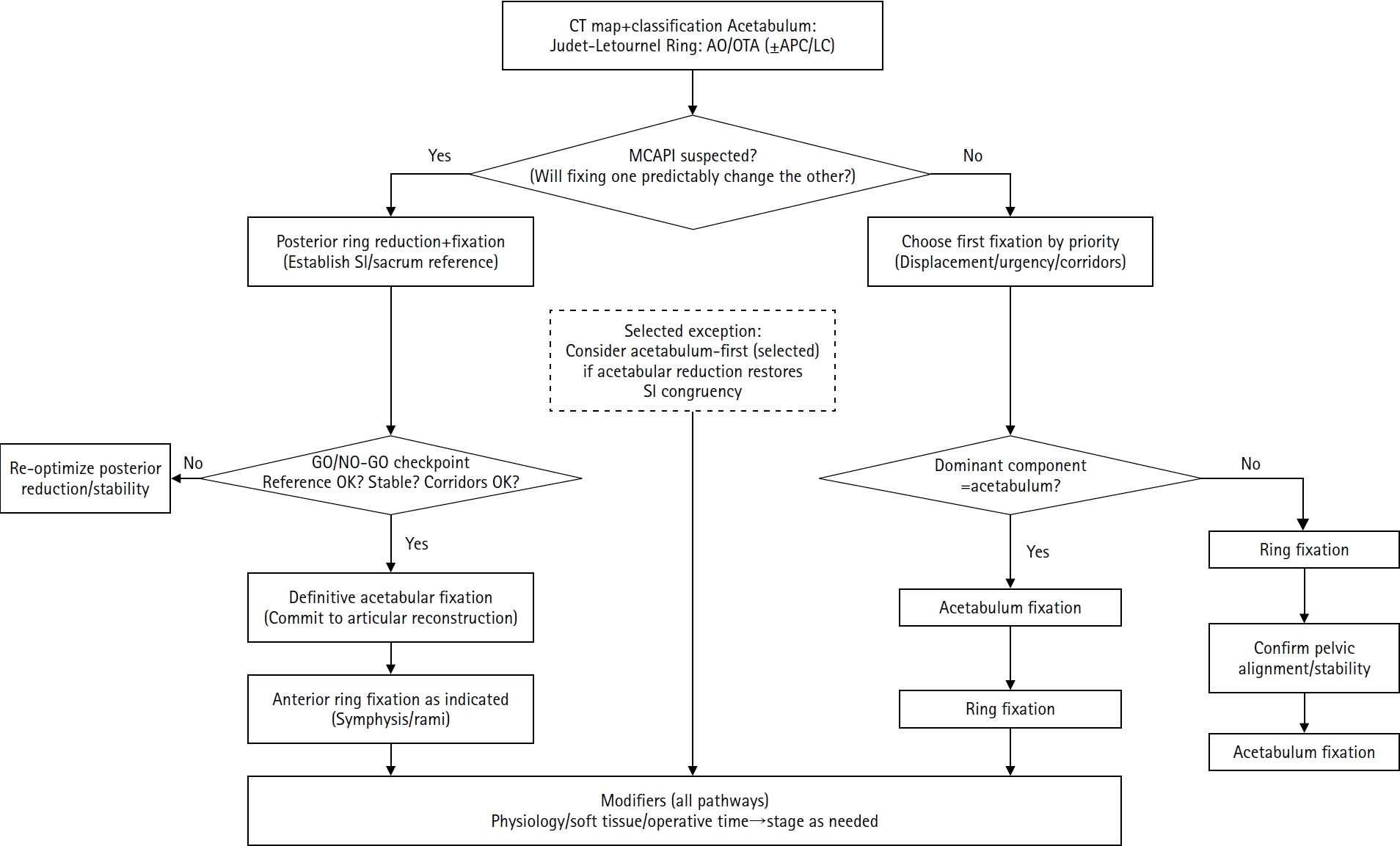
Reference-frame algorithm for definitive fixation sequencing in combined pelvic ring and acetabular injuries.
| Study (yr) | Design | No./scope | Definition/inclusion (as used) | Classification | Sequencing/strategy (key message) | Outcome highlights | Complications/risk signals |
|---|---|---|---|---|---|---|---|
| Halvorson et al. 2014 [4] | Narrative review | Evidence synthesis | Combined acetabular fracture with pelvic ring injury; definitions vary across series | Judet-Letournel ring described with OTA/Young-Burgess concepts | Integrated planning based on mechanical interaction identifies scenarios where acetabular fixation facilitates SI joint reduction | Higher injury burden (ISS) and morbidity than isolated fracture patterns | Emphasizes multidisciplinary care and physiological optimization to manage systemic morbidity |
| Veerappa et al. 2020 [6] | Systematic review (PRISMA) | 8 Retrospective series (≥20 cases) | Combined pelvic and acetabular injuries (heterogeneous definitions) | Lack of standardized terminology | Consensus-based sequencing: reinforces “ring first” standard (posterior → acetabulum → anterior) based on pooled series | Reported incidence: 5%–16% of pelvic/acetabular injuries; transverse and both-column patterns are most frequent | Confirms that heterogeneous definitions and a lack of standardized terminology limit strong comparative conclusions |
| Ross et al. 2023 [5] | Systematic review (PRISMA) | 11 Series (985 patients) | Combined pelvic ring + acetabular fractures (ipsilateral/contralateral included) | Lack of standardized terminology | Sequencing remains debated; unstable rings are often managed with ring first logic; acetabular reduction quality is emphasized | Across studies: mean ISS ~23; pooled mortality ~8%; functional metrics inconsistently reported | Calls for standardized definitions, radiographic metrics, and PROMs |
| Puchwein et al. 2024 [2] | State-of-the-art review | Algorithmic framework | Emphasizes mechanically connected patterns (MCAPI) vs. less connected combinations | Judet-Letournel (acetabulum) + AO/OTA (ring); APC/LC as adjunct | For MCAPI: pelvic ring first (sacrum/SI joint) is generally favored; acetabulum-first is reserved for selected cases with stable posterior rings | Definitive fixation within an early window (~3 to 7 days) is ideal, subject to physiologic and soft-tissue status | Temporary stabilization pitfalls: inadequate initial stability can compromise definitive reduction; emphasize planning for complex coupling |
| Suzuki et al. 2010 [12] | Retrospective cohort (Level I) | 82 Combined (68 operative) | Unstable pelvic injury plus displaced acetabular fracture treated at a Level I center | OTA/Young-Burgess (ring); OTA acetabulum descriptors | Reference-frame principle: prioritizes posterior ring reduction to establish a stable foundation before articular fixation | Mean time to surgery: 5.7 days; | Residual posterior pelvic displacement is a significant predictor of poor acetabular reduction quality |
| Mean postoperative acetabular displacement: 2.2 mm | |||||||
| Osgood et al. 2013 [1] | Retrospective pattern study | 40 Combined (institutional database) | Combined pelvic ring disruption + acetabular fracture identified from institutional registry | Young-Burgess (ring); Letournel (acetabulum) | Morphological mapping: defines common injury combinations, providing a basis for initial planning and corridor assessment | Distribution: APC (53%), LC (45%), VS (3%); | High systemic injury burden: mortality rate of ~13%, characterized by high ISS and frequent associated injuries |
| Posterior wall fractures are significantly less common (~5%) than in isolated cohorts | |||||||
| Cai et al. 2017 [10] | Retrospective case series | 21 Operative | Unstable pelvic fractures with concomitant acetabular fractures are managed operatively | Tile (pelvis) & Letournel (acetabulum) approach- and fixation-based reporting; Matta and functional scores used | Individualized planning: focuses on patient-specific surgical approach and corridor selection when a standardized sequence is not applicable | Functional success: Majeed excellent/good in 85.7% (18/21) at final follow-up | Reports specific complications, including heterotopic ossification, femoral head necrosis, and iatrogenic neurovascular injury |
| Li et al. 2023 [17] | Retrospective case series | 24 Tile B/C | Unstable pelvic fractures combined with acetabular fractures (single center) | Tile (ring); Judet-Letournel (acetabulum) | Posterior-first preference: emphasizes stabilizing posterior ring alignment to provide a reliable template for complex acetabular reconstruction | High functional success: Majeed excellent/good (87.5%) and Merle d’Aubigne excellent/good (83.3%) at final follow-up | Reinforces that anatomic restoration through morphology-based sequencing yields favorable long-term functional results |
| Cunningham et al. 2023 [16] | Retrospective risk-factor study | 70 (≥1-yr follow-up) | Operatively treated combined ring + acetabulum injuries (single Level I center) | Not classification-driven; focuses on predictors of complications | Percutaneous acetabular methods are associated with fewer complications than open approaches | Overall complication rate: 44%; | Hip dislocation is a major predictor of all-cause complications and residual neurologic deficits; angio/embolization is not linked to deep infection |
| Hip dislocation incidence: 40% | |||||||
| Fratus et al. 2025 [13] | Retrospective comparative cohort | 45 (posterior-first vs. others) | Adults requiring operative management; excluded are stable ring/nonoperative acetabulum/nondisplaced percutaneous acetabulum | Postoperative CT step-off and gapping endpoints | Posterior-first preference: validates that addressing the posterior ring first leads to superior anatomic reduction of the acetabulum on CT | CT-based endpoints: anatomic step-off (68.2% vs. 30.4%) and gapping (27.3% vs. 4.4%) significantly favor the posterior-first approach | Reinforces reduction quality but notes that correlation with long-term PROMs remains uncertain |
Definitions and outcomes vary across studies; this table summarizes dominant decision points and sequencing signals rather than prescribing a single universal protocol.
OTA, Orthopedic Trauma Association; ISS, injury severity score; PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-analyses; PROM, patient-reported outcome measure; MCAPI, mechanically connected acetabular and pelvic ring injuries (working framework); AO/OTA, Arbeitsgemeinschaft für Osteosynthesefragen/Orthopedic Trauma Association; APC/LC/VS, anteroposterior compression/lateral compression/vertical shear (Young-Burgess); SI joint, sacroiliac joint; CT, computed tomography;
- 1. Osgood GM, Manson TT, O'Toole RV, Turen CH. Combined pelvic ring disruption and acetabular fracture: associated injury patterns in 40 patients. J Orthop Trauma 2013;27:243-7.ArticlePubMed
- 2. Puchwein P, Sandersjoo G, Lindahl J, Eibinger N. Combined pelvic ring and acetabular fractures: strategies and sequence of surgery. State of the art. Arch Orthop Trauma Surg 2024;144:4577-86.ArticlePubMedPMCPDF
- 3. Gänsslen A, Pohlemann T, Paul C, Lobenhoffer P, Tscherne H. Epidemiology of pelvic ring injuries. Injury 1996;27 Suppl 1:S-A13-20.ArticlePubMed
- 4. Halvorson JJ, Lamothe J, Martin CR, et al. Combined acetabulum and pelvic ring injuries. J Am Acad Orthop Surg 2014;22:304-14.ArticlePubMed
- 5. Ross H, Stine S, Blue K, Wolterink TD, Vaidya R. Systematic review of combined pelvic ring and acetabular injuries: what do we know from the literature? Cureus 2023;15:e41843. ArticlePubMedPMC
- 6. Veerappa LA, Tippannavar A, Goyal T, Purudappa PP. A systematic review of combined pelvic and acetabular injuries. J Clin Orthop Trauma 2020;11:983-8.ArticlePubMedPMC
- 7. Burgess AR, Eastridge BJ, Young JW, et al. Pelvic ring disruptions: effective classification system and treatment protocols. J Trauma 1990;30:848-56.PubMed
- 8. Judet R, Judet J, Letournel E. Fractures of the acetabulum: classification and surgical approaches for open reduction. Preliminary report. J Bone Joint Surg Am 1964;46:1615-46.PubMed
- 9. Letournel E. Acetabulum fractures: classification and management. Clin Orthop Relat Res 1980;81-106.Article
- 10. Cai L, Lou Y, Guo X, Wang J. Surgical treatment of unstable pelvic fractures with concomitant acetabular fractures. Int Orthop 2017;41:1803-11.ArticlePubMedPDF
- 11. Porter SE, Schroeder AC, Dzugan SS, Graves ML, Zhang L, Russell GV. Acetabular fracture patterns and their associated injuries. J Orthop Trauma 2008;22:165-70.ArticlePubMed
- 12. Suzuki T, Smith WR, Hak DJ, et al. Combined injuries of the pelvis and acetabulum: nature of a devastating dyad. J Orthop Trauma 2010;24:303-8.ArticlePubMed
- 13. Fratus A, Nirunsuk P, Tucker NJ, Parry JA, Mauffrey C. Combined pelvic and acetabular injuries: Decision making and clinical results. Injury 2025;56:112364.ArticlePubMed
- 14. Gansslen A, Lindahl J, Krappinger D, Lindtner RA, Staresinic M. Outcome of pelvic ring injuries. Arch Orthop Trauma Surg 2024;145:47.ArticlePubMedPMC
- 15. Mauffrey C, Bellas N, David G, Le Baron M. Understanding acetabular fractures: a comprehensive review. J Am Acad Orthop Surg 2025 Dec 22 [Epub]. https://doi.org/10.5435/JAAOS-D-25-00741. Article
- 16. Cunningham B, Pearson J, McGwin G, et al. What are the risk factors for complications after combined injury of the pelvic ring and acetabulum? Eur J Orthop Surg Traumatol 2023;33:341-6.ArticlePubMedPDF
- 17. Li R, Zhao P, Guan J, Wang X, Liu L, Wu M. Combined pelvic, acetabular injuries: clinical features and treatment strategies of a unique injury pattern. J Orthop Surg Res 2023;18:415.ArticlePubMedPMC
- 18. Marchand LS, Sepehri A, Hannan ZD, et al. Pelvic ring injury mortality: are we getting better? J Orthop Trauma 2022;36:81-6.ArticlePubMedPMC
- 19. Cuthbert R, Walters S, Ferguson D, et al. Epidemiology of pelvic and acetabular fractures across 12-mo at a level-1 trauma centre. World J Orthop 2022;13:744-52.ArticlePubMedPMC
References
Figure & Data
REFERENCES
Citations

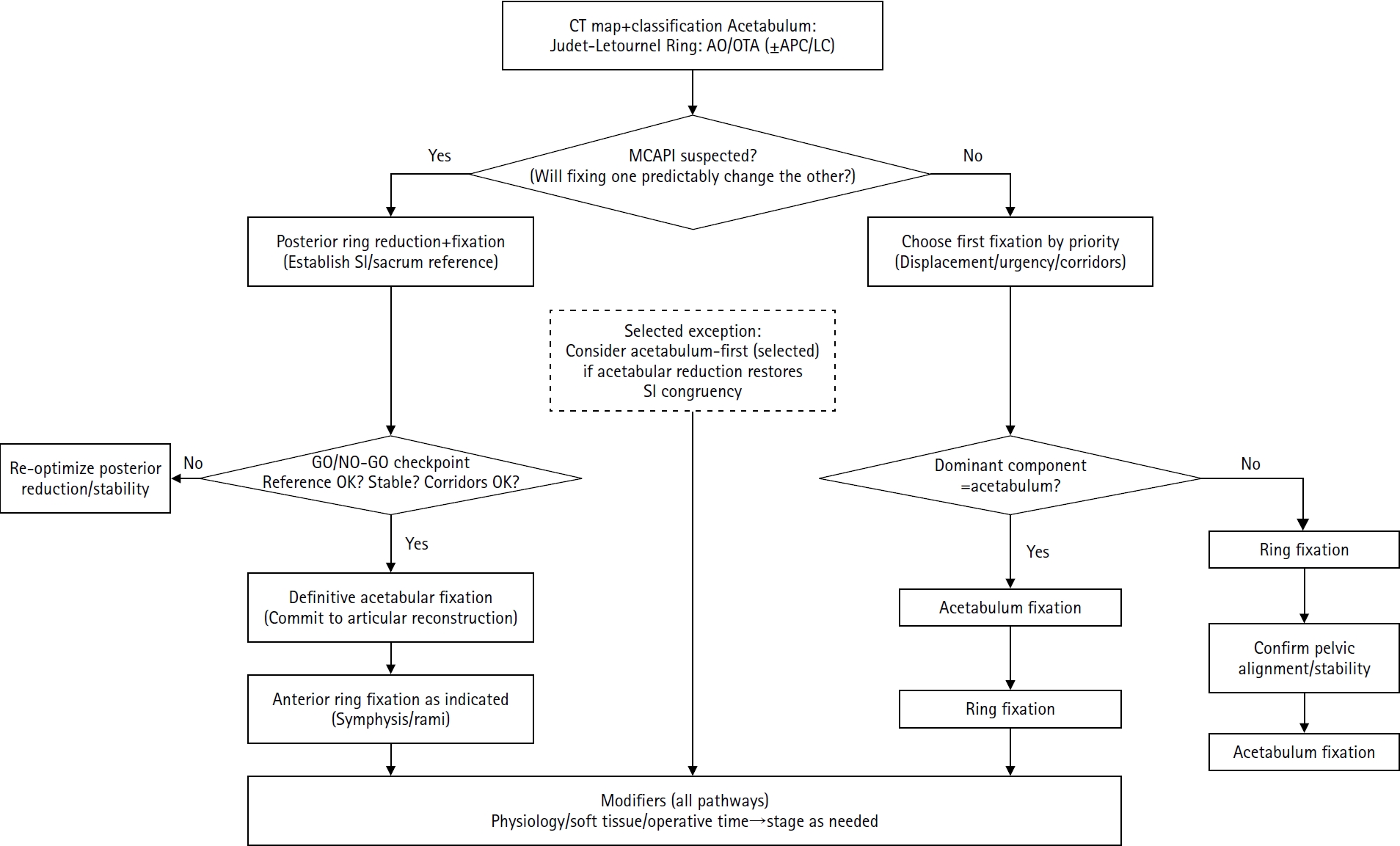
Fig. 1.
| Study (yr) | Design | No./scope | Definition/inclusion (as used) | Classification | Sequencing/strategy (key message) | Outcome highlights | Complications/risk signals |
|---|---|---|---|---|---|---|---|
| Halvorson et al. 2014 [4] | Narrative review | Evidence synthesis | Combined acetabular fracture with pelvic ring injury; definitions vary across series | Judet-Letournel ring described with OTA/Young-Burgess concepts | Integrated planning based on mechanical interaction identifies scenarios where acetabular fixation facilitates SI joint reduction | Higher injury burden (ISS) and morbidity than isolated fracture patterns | Emphasizes multidisciplinary care and physiological optimization to manage systemic morbidity |
| Veerappa et al. 2020 [6] | Systematic review (PRISMA) | 8 Retrospective series (≥20 cases) | Combined pelvic and acetabular injuries (heterogeneous definitions) | Lack of standardized terminology | Consensus-based sequencing: reinforces “ring first” standard (posterior → acetabulum → anterior) based on pooled series | Reported incidence: 5%–16% of pelvic/acetabular injuries; transverse and both-column patterns are most frequent | Confirms that heterogeneous definitions and a lack of standardized terminology limit strong comparative conclusions |
| Ross et al. 2023 [5] | Systematic review (PRISMA) | 11 Series (985 patients) | Combined pelvic ring + acetabular fractures (ipsilateral/contralateral included) | Lack of standardized terminology | Sequencing remains debated; unstable rings are often managed with ring first logic; acetabular reduction quality is emphasized | Across studies: mean ISS ~23; pooled mortality ~8%; functional metrics inconsistently reported | Calls for standardized definitions, radiographic metrics, and PROMs |
| Puchwein et al. 2024 [2] | State-of-the-art review | Algorithmic framework | Emphasizes mechanically connected patterns (MCAPI) vs. less connected combinations | Judet-Letournel (acetabulum) + AO/OTA (ring); APC/LC as adjunct | For MCAPI: pelvic ring first (sacrum/SI joint) is generally favored; acetabulum-first is reserved for selected cases with stable posterior rings | Definitive fixation within an early window (~3 to 7 days) is ideal, subject to physiologic and soft-tissue status | Temporary stabilization pitfalls: inadequate initial stability can compromise definitive reduction; emphasize planning for complex coupling |
| Suzuki et al. 2010 [12] | Retrospective cohort (Level I) | 82 Combined (68 operative) | Unstable pelvic injury plus displaced acetabular fracture treated at a Level I center | OTA/Young-Burgess (ring); OTA acetabulum descriptors | Reference-frame principle: prioritizes posterior ring reduction to establish a stable foundation before articular fixation | Mean time to surgery: 5.7 days; | Residual posterior pelvic displacement is a significant predictor of poor acetabular reduction quality |
| Mean postoperative acetabular displacement: 2.2 mm | |||||||
| Osgood et al. 2013 [1] | Retrospective pattern study | 40 Combined (institutional database) | Combined pelvic ring disruption + acetabular fracture identified from institutional registry | Young-Burgess (ring); Letournel (acetabulum) | Morphological mapping: defines common injury combinations, providing a basis for initial planning and corridor assessment | Distribution: APC (53%), LC (45%), VS (3%); | High systemic injury burden: mortality rate of ~13%, characterized by high ISS and frequent associated injuries |
| Posterior wall fractures are significantly less common (~5%) than in isolated cohorts | |||||||
| Cai et al. 2017 [10] | Retrospective case series | 21 Operative | Unstable pelvic fractures with concomitant acetabular fractures are managed operatively | Tile (pelvis) & Letournel (acetabulum) approach- and fixation-based reporting; Matta and functional scores used | Individualized planning: focuses on patient-specific surgical approach and corridor selection when a standardized sequence is not applicable | Functional success: Majeed excellent/good in 85.7% (18/21) at final follow-up | Reports specific complications, including heterotopic ossification, femoral head necrosis, and iatrogenic neurovascular injury |
| Li et al. 2023 [17] | Retrospective case series | 24 Tile B/C | Unstable pelvic fractures combined with acetabular fractures (single center) | Tile (ring); Judet-Letournel (acetabulum) | Posterior-first preference: emphasizes stabilizing posterior ring alignment to provide a reliable template for complex acetabular reconstruction | High functional success: Majeed excellent/good (87.5%) and Merle d’Aubigne excellent/good (83.3%) at final follow-up | Reinforces that anatomic restoration through morphology-based sequencing yields favorable long-term functional results |
| Cunningham et al. 2023 [16] | Retrospective risk-factor study | 70 (≥1-yr follow-up) | Operatively treated combined ring + acetabulum injuries (single Level I center) | Not classification-driven; focuses on predictors of complications | Percutaneous acetabular methods are associated with fewer complications than open approaches | Overall complication rate: 44%; | Hip dislocation is a major predictor of all-cause complications and residual neurologic deficits; angio/embolization is not linked to deep infection |
| Hip dislocation incidence: 40% | |||||||
| Fratus et al. 2025 [13] | Retrospective comparative cohort | 45 (posterior-first vs. others) | Adults requiring operative management; excluded are stable ring/nonoperative acetabulum/nondisplaced percutaneous acetabulum | Postoperative CT step-off and gapping endpoints | Posterior-first preference: validates that addressing the posterior ring first leads to superior anatomic reduction of the acetabulum on CT | CT-based endpoints: anatomic step-off (68.2% vs. 30.4%) and gapping (27.3% vs. 4.4%) significantly favor the posterior-first approach | Reinforces reduction quality but notes that correlation with long-term PROMs remains uncertain |
Definitions and outcomes vary across studies; this table summarizes dominant decision points and sequencing signals rather than prescribing a single universal protocol. OTA, Orthopedic Trauma Association; ISS, injury severity score; PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-analyses; PROM, patient-reported outcome measure; MCAPI, mechanically connected acetabular and pelvic ring injuries (working framework); AO/OTA, Arbeitsgemeinschaft für Osteosynthesefragen/Orthopedic Trauma Association; APC/LC/VS, anteroposterior compression/lateral compression/vertical shear (Young-Burgess); SI joint, sacroiliac joint; CT, computed tomography;

 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

